Shape
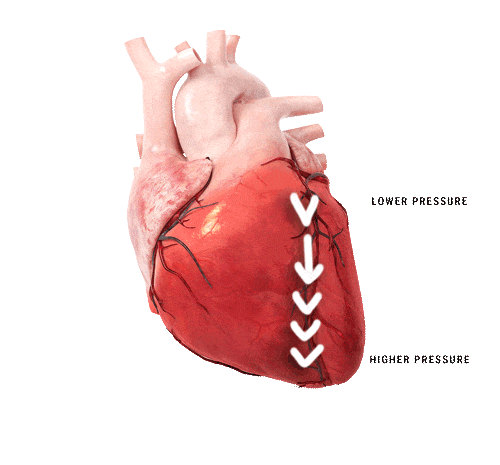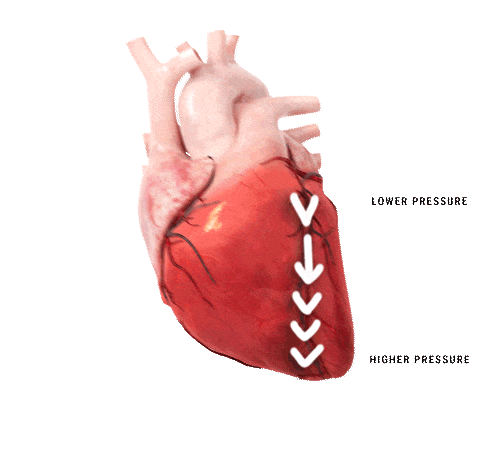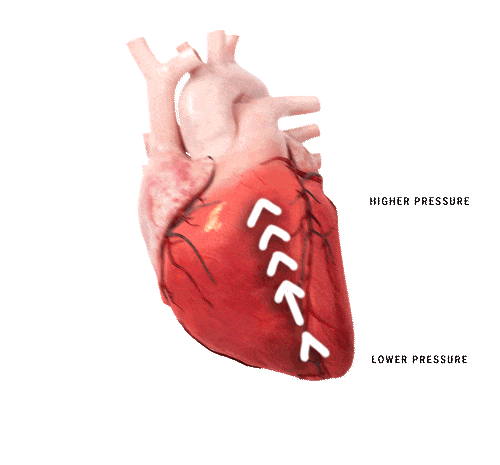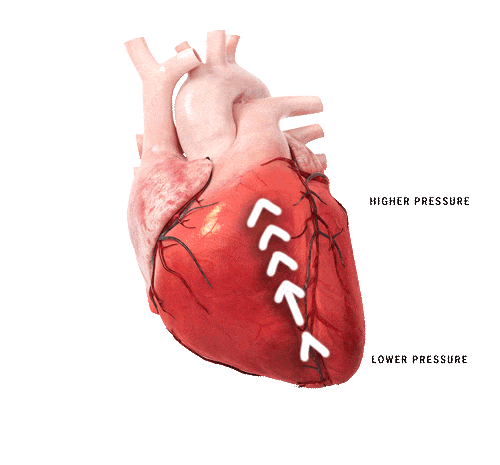
The shape of the heart contributes to generating blood flow towards the outflow tract during contraction. A change in shape, deformation, either regionally or globally, results in a different contraction pattern which may lead to a change in its functional power. The volumetric output can still be the same as in a healthy heart, however it costs the heart more energy to compensate for the change in contraction pattern. By detecting either global or regional deformation, prediction of major adverse cardiovascular events (MACE) becomes possible. This holds incremental prognostic information for the patients.